Pressure Sores, Pressure Ulcers, Decubitus Ulcers, Or Bed Sores
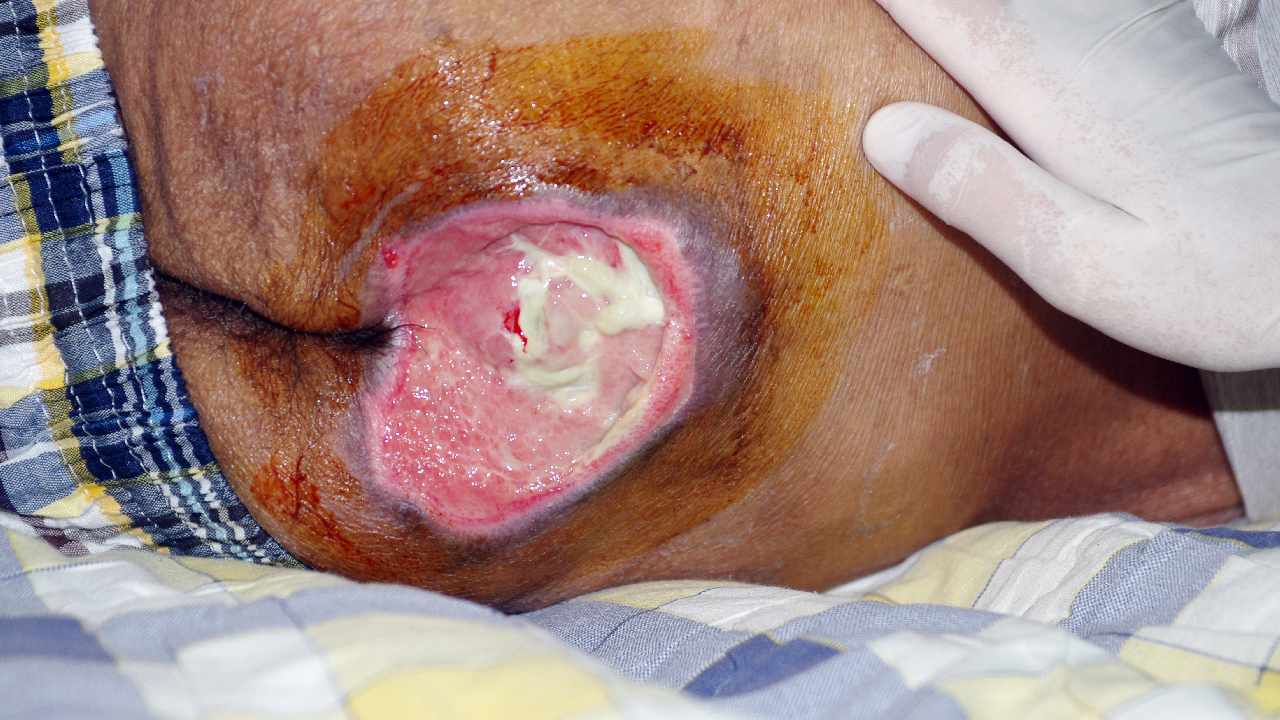
Many names are used for sores that can develop over a bony pressure area, such as the coccyx, hip, heel, shoulder, elbow, and back of the head. These ulcers tend to be painful, cause misery and suffering, infection, reduce the quality of life, or even result in early death.
While most often called “Pressure Ulcers,” frequently other names are recorded in the medical records. These ulcers often develop because the nursing standard of care and other professional standards in a facility has not been followed. But once developed, treatment of these ulcers is costly and requires significant time and multidisciplinary staff to heal.
The Agency for Healthcare Research & Quality (AHRQ) estimates more than 2.5 million individuals in the US develop pressure ulcers annually,[1] at an enormous cost to the US Health Care System.
It has been averaged that pressure sores cost between $9.1 billion to $11.6 billion per year. There have been numerous lawsuits and much time and energy spent on something avoidable for the most part.
Areas to Review
When reviewing medical records, it is essential to determine why these ulcers occurred. Was the ulcer avoidable? Were there deviations in the nursing standard of care? Did the resident develop a pressure ulcer but should not have?
Listed below are some areas to review, including but not limited to, the following:
- Evaluation of the clinical condition and risk factor for pressure sores, such as using a prediction risk tool such as the Braden Scale[2].
- Interventions were implemented consistent with the resident needs and goals, such as turning and repositioning, appropriate pressure relief, and/or alternating air bed provided on the care plan.
- Was the resident monitored and regularly evaluated for any changes?
- Did the resident receive the nutritional needs per the dietary assessment?
- Were activities of daily living of toileting, bathing, and repositioning provided?
- Proper skincare for the prevention of skin breakdown?
- Lifting and transfer assessed and provided per the standard of care?
- Did the resident sit in the wheelchair for long periods, not toileted, not kept clean and dry?
- Was the care plan developed to include all the nursing interventions?
- Did the staff follow the plan of care?
- Were appropriate interventions for prevention care planned and revised as needed?
A pressure ulcer is any sore caused by unrelieved pressure in a particular area on the body, resulting in damage to the tissue(s). Friction and shearing are not always a primary cause of pressure ulcers, but this can damage the tissues, increasing the risk factor for further damage such as a pressure sore.
Sometimes a facility will say that the pressure ulcer is “unavoidable.” In the review of the medical records, were all the clinical conditions and risk factors assessed? It’s essential to review if the staff provided all the necessary interventions and if the standard of practice was provided?
Federal Standards
Based on federal Standard 42 CFR 483.25 (b)(1) related to pressure ulcers, the facility must ensure that…
- A resident receives care consistent with professional standards of practice to prevent pressure ulcers and does not develop pressure ulcers unless the individual’s clinical condition demonstrates that they were unavoidable; and
- A resident with pressure ulcers receives necessary treatment and services, consistent with professional standards of practice, to promote healing, prevent infection, and prevent new ulcers from developing.[3]
This requirement intends that the resident does not develop pressure ulcers unless clinically unavoidable. The facility must provide care to promote prevention and promote healing if any are present. This includes patients admitted with an ulcer; the facility must prevent the development of additional pressure ulcers.[4]
In my professional experience and opinion, very rarely, if at all, should pressure ulcers develop when the nursing staff and facility provide the nursing standard of care and other professional standards. However, if ulcers do occur, they should be reviewed to determine if there was abuse or neglect?
There is important information from the Federal government and other agencies for the prevention and if developed or admitted to the facility with a pressure ulcer. There are many treatment options for complete healing. Certified wound care health providers are available to be part of the team to provide prevention assessments, care plans, and treatments if necessary.
There is further information regarding Long Term Care facilities on Medicare.gov. Check out Nursing Home Compare http://www.medicare.gov/nursinghomecompare This is a site to be included in your overall review of a facility to obtain information.
[1] https://www.o-wm.com/article/pressure-ulcers-united-states-inpatient-population-2008-2012-results-retrospective
[2] https://en.wikipedia.org/wiki/Braden_Scale_for_Predicting_Pressure_Ulcer_Risk
[3] https://www.govregs.com/regulations/42/483.25
[4] https://nursinghome411.org/wp-content/uploads/2019/04/LTCCC-Pressure-Ulcer-Fact-Sheet.pdf
NURSE EXPERT SOLUTIONS
How To Use Your Knowledge And Experience To Start A Nurse Expert Business Today...
Work from home, set your own hours, and generate more income for your family
Here Is What You Get Inside "Nurse to Expert: Your Complete Transformation Blueprint"
- You get immediate, 24/7, unlimited lifetime access to the "Nurse to Expert: Your Complete Transformation Blueprint" program so you can study the material whenever and wherever you want.
- You get instant access to all nine-course modules. All videos are short, bite-sized, and easy to consume, so you can get through the content even if you don’t have much time.
- You get immediate access to all supporting documents: spreadsheets, PDFs, and other resource files; download and customize them to fit your business.
- You get instant access to all three Bonus Case Studies where I walk you through real-life cases and scenarios so that you understand the “Nurse to Expert: Your Complete Transformation Blueprint” process.

